Photo Credit: mheim3011 / iStockPhoto.com
What Is Leaky Gut and How Do I Know If I Have It?
The concept of a leaky gut is relatively new to mainstream science. It is not a disease taught in medical school; it is, however, diagnosed in alternative medicine. While leaky gut remains controversial as a disease entity in itself, there is more and more evidence emerging about the association between leaky gut and certain diseases.
While leaky gut remains controversial as a disease entity in itself, there is more and more evidence emerging about the association between leaky gut and certain diseases.
Defining Leaky Gut
Gut leakiness refers to the degree of permeability of the intestinal wall. The walls of the intestine have a very important role.
As far as the body is concerned, the insides of the intestine are foreign; filled with bacteria and microorganisms and food and potential toxins and foreign plant materials, dirt and dust. The walls of the intestine serve as a very important barrier and gateway into the body.
On the one hand, they need to selectively let nutrients in, yet on the other hand, they must keep harmful substances out. Even in a normal functioning gut, the physical barrier isn’t perfect. To compensate, the intestinal walls are filled with inflammatory cells ready to attack invading microorganisms, and there is a lymphatic network that directs absorbed substances to the liver where toxins can be filtered out.
The lining of the intestinal wall consists of a single contiguous layer of cells joined together very tightly by protein bridges, called tight junctions. There are gates and channels that selectively let nutrients in, through and between these cells.
Underneath these cells are more cells, regularly stepping up to take their place as they get injured or die. Replacement must be carefully coordinated to prevent leakage of intestinal contents as the cells turnover. Defects in the junctions between cells can lead to the intestines becoming leaky, allowing potentially harmful substances, foreign materials, incompletely digested nutrients and microorganisms to enter the body through gaps between the cells of the intestinal wall.
If foreign or toxic materials cross the intestinal wall barrier uninvited they can cause inflammation, not only locally but also elsewhere in the body. This is similar to patients with a severe dental disease, where the bacteria in the mouth not only cause local inflammation but they also enter the bloodstream and can cause kidney disease, heart disease and even reduce fertility.
If you have ever felt like the world is spinning around you, or that you are spinning yourself, you may suffer from vertigo.
Similarly, increased intestinal permeability has been linked to kidney inflammation, cardiovascular disease, migraines, mood, cancer, autism, chronic fatigue syndrome and autoimmune disease. The difficulty for doctors is working out what is the cause and what is effect.
The intestinal walls amount to a lot of surface area — approximately half a badminton court. That is a lot of area where things could go wrong. Science is only beginning to understand the true nature of the structures that hold the cells of the intestinal wall tightly together.
The proteins involved come with names of the type claudin-, occludin-, zonulin- and cadherin-. Research is emerging that mutations and defects in these proteins may contribute to numerous diseases by increasing permeability of the intestinal wall.
Crohn’s disease, for example, has been linked to defects in the protein N-cadherin. Some bacteria and viruses even deliberately target these proteins, increasing gut permeability presumably to help their growth and spread.
With a leaky gut, the body is not only exposed to bacteria but also to incompletely digested substances and foreign particles, which it recognizes as foreign. This triggers an immune response. In some instances, in the context of a predisposed immune system, these foreign substances may trick the body into attacking parts of itself.
Links to Other Diseases
This is a relatively new theory regarding the development of a number of autoimmune and inflammatory diseases, such as type I diabetes. In the context of abnormal intestinal permeability, exposure to an as yet unknown foreign agent triggers the immune system to attack the cells of the pancreas responsible for insulin production.
Other autoimmune diseases linked to a leaky gut include irritable bowel syndrome, celiac disease, multiple sclerosis, autoimmune hepatitis and rheumatoid arthritis.
It is recognized that many disorders have concurrent increased intestinal permeability. Dietary modifications aimed at improving a leaky gut have benefited some people experiencing it.
What does this new knowledge of leaky guts mean for the general public — for those that suffer from unexplained intestinal symptoms? Might some people have a defect in one of the proteins that hold the intestinal cells together?
Indeed, some relatives of Crohn’s disease sufferers have increased intestinal permeability with non-symptomatic intestinal inflammation. This indicates that individuals with non-overt disease but with leaky guts exist in the population. Certainly, leaky gut is in need of more research.
Symptoms and Testing for Leaky Gut
Numerous lifestyle factors are known to increase intestinal permeability. These include energy-rich diets, alcohol, stress, infections, inflammation and certain medications.
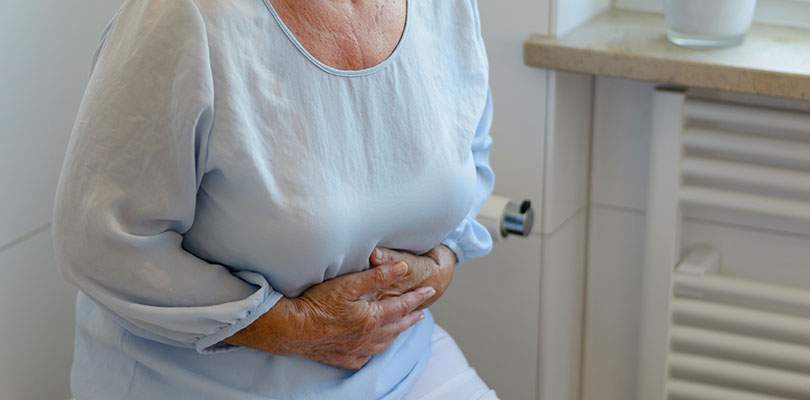
Symptoms of a leaky gut are related to local inflammation of the intestines and include abdominal pain, bloating, excess gas, increased food sensitivities and chronic diarrhea or constipation. More widespread effects might include general aches and pains.
There is no bedside clinical test for checking intestinal permeability. If you have intestinal symptoms and your doctor has ruled out other common causes, consider that you might have a leaky gut. Try a change in diet. Avoid factors that increase gut permeability and try probiotics. After all, it has been shown to help in people with certain autoimmune diseases.