Krystina's Meningioma Story
About a year and a half ago, I got a phone call that stopped me in my tracks.
I was in my living room, doing yoga.
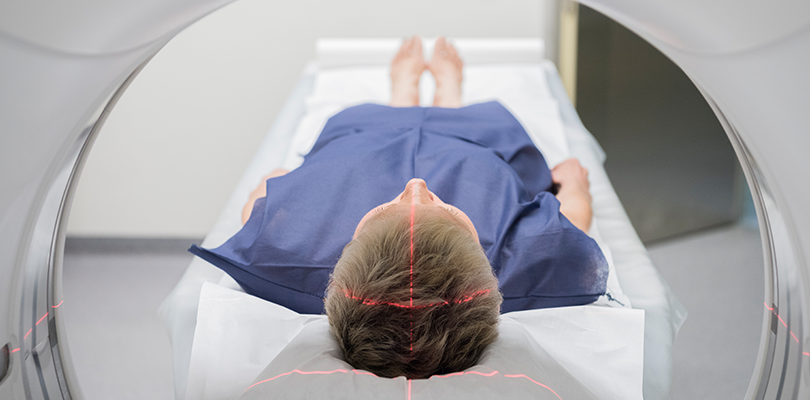
About a week before, I had an MRI done for increasing migraines. I’d had MRIs done in the past, all of which had negative findings.
"Hello, is this Krysti? Hi, this is Dr. Johnson’s nurse. Dr. Johnson* wanted me to call and let you know your MRI came back fine. There was, however, an incidental finding of a small meningioma. He said we could just talk about it at your next appointment."
I didn’t think anything about this as I hung up the phone. In fact, I continued doing yoga. Then five minutes later, I realized, "What is a meningioma?"
A quick Google search showed me that a meningioma is a brain tumor. Let the panic ensue.
*The name of the doctor has been changed.
What is a Meningioma?
A meningioma is a tumor that forms on the outermost covering of the brain and spinal cord, the meninges.
The meninges can be further broken down into the dura mater, the arachnoid, and the pia mater, with the meningioma originating in the arachnoid layer and growing outward.
These tumors grow on the meninges and grow inward. When they grow inward, they typically do not invade the brain’s soft tissue, but they do invade space in the brain.
Meningiomas are usually benign, although some are cancerous. Meningiomas are typically extremely slow-growing tumors, which is why many people do not know they have them until they grow large enough to cause extreme symptoms.
Meningioma Statistics and Facts
- Depending on the source, meningiomas account for 20-37 percent of all brain tumors and account for 10% of all tumors of the spine.
- It's estimated that 27,110 people will be diagnosed with a meningioma in 2017.
- 90% of meningiomas are benign; the remaining 10% are either atypical or malignant. An atypical meningioma means the tumor is neither benign nor malignant but may become cancerous.
- Meningiomas are much more likely to occur in women – there is a female to male ratio of 3:1 in the brain and 6:1 in the spinal cord.
- Meningiomas almost exclusively occur in adults – pediatrics represent only 1.5% of cases.
Who Gets Diagnosed With Meningiomas?
Women are much more likely to get meningiomas than men or children, and individuals who are between the ages of 40 and 70 are much more likely to be diagnosed with a meningioma.
There are also other risk factors:
- Previous exposure to radiation treatment, or nuclear radiation.
- A blow to the skull.
- Genetic predisposition – people who have a genetic disorder called neurofibromatosis 2 (Nf2) have a greater likelihood of developing meningiomas. Their tumors are also more likely to be malignant.
- Some tumors can also be estrogen-sensitive, meaning that extra estrogen in the body can make them grow.
Proper oral hygiene can mean more than just having a great smile. In fact, it may be the one thing standing between you and common oral health problems.
Treatment Options For Meningiomas
When I saw a neurosurgeon, she discussed my treatment options with me about my small tumor.
As a result, we had no way of knowing when the meningioma formed, if it was growing, and how it would be monitored. We opted with serial MRIs with intervention taking place when needed.
Watch and Wait
The watch and wait treatment involves serial MRIs to be performed in a specific amount of time to monitor the growth of the tumor.
For that reason, my watch & wait schedule went as the following:
- An MRI, three months after diagnosis.
- A CT scan, six months after diagnosis.
- And then an MRI one year after diagnosis.
Above all, depending on your neurosurgeon, many have different "schedules" for the watch & wait option.
Resection
This essentially means removal of the tumor. Resection surgery is performed when imaging has detected a pattern of growth or when symptoms have warned removal of the tumor.
The most common way to remove a meningioma is by craniotomy. A craniotomy involves removing a tiny portion of the skull to remove the tumor, then placing the skull flap back and suturing it together.
However, depending on the many different areas of the brain where a meningioma can occur, there are also minimally invasive types of surgeries that can be performed. Your surgeon will discuss with you further about the options for surgery.
Radiation
When we hear the term “radiation” we probably don’t realize that there are a variety of different types available – primarily to treat tumors of the head.
This treatment modality is an attractive option for people with meningioma that are inoperable or who do not want to have surgery.
There also may be instances where a physician may prefer radiation over surgery for certain individuals as radiation involves using high-energy x-rays to destroy the tumor cells.
What’s Next for Me?
I’m heading to Mayo Clinic in about six weeks for a resection of my meningioma.
At the Mayo Clinic, my tumor was found to be growing, or as the radiation oncologist told me, “It is biologically active!” As I am young and the tumor is in an easily operable area, I’ve elected to have it removed completely.
Once the tumor is removed, it will be sent to pathology, where it will be tested for malignancy. It will also be tested to see if it is an estrogen-receptive tumor, due to my age, and other related tests they deem is necessary to check.
I’ll have a follow-up article discussing my surgery and recovery, and actionable steps that you can take if you're presented the opportunity for elective surgery.