Deep Vein Thrombosis Symptoms Explained
Blood clots can lead to serious health issues. It’s important to know potential complications if you are susceptible to blood clotting. Certain medical conditions need immediate attention, and deep vein thrombosis (DVT) is one of them. In order to catch this condition, it is good to know about deep vein thrombosis symptoms.
What Is Deep Vein Thrombosis?
DVT is a major health concern that can cause long lasting health problems and potentially be life threatening. A thrombus is a blood clot and DVT is a blood clot that occurs in a deep vein, usually in the legs.
DVT can occur in the arms as well, but this is much rarer than in the legs. A DVT clot can damage the vein and cause pain in the leg, as well as swelling. The danger with DVT is that parts of the clot can break loose, traveling through the bloodstream and into the lungs. If a clot reaches the lungs, it can block blood flow and result in a pulmonary embolism, which is usually life threatening. The chance of dying from a pulmonary embolism is over 25%, so urgent medical care is vital.
Causes of Deep Vein Thrombosis
Blood clots form in superficial and deep veins and often form in the arms or pelvic veins. Clots in superficial veins that cause inflammation do not usually cause serious problems. Blood clots form in veins from inactivity and immobility causes blood to pool and clot in the legs. DVT is caused by anything that prevents your blood from circulating or clotting normally, which is why it is fundamental to move your body as often as possible. Damage to the deep veins make clotting more likely, so something like surgery or an injury can harm blood vessels and create a blood clot. Other causes of DVT include:
- Being paralyzed or bedridden
- A family history with DVT, pulmonary embolism, blood clotting disorder, or other inherited genetic conditions which increase clotting
- Certain medical conditions can affect how your blood clots
- Sitting for a long flight or car trip
- Some forms of cancer and cancer treatment
- Heart failure
Risk Factors for Deep Vein Thrombosis
There are some risks associated with DVT other than immobility. The following may increase your risk of getting DVT:
- Being overweight, as it increases pressure in the veins in your pelvis and legs
- Smoking, as it affects blood clotting and circulation
- A personal history of past DVT
- Inflammatory bowel disease
- Being older than 60
- Birth control pills or hormone replacement therapy
- Pregnancy
Symptoms of Deep Vein Thrombosis
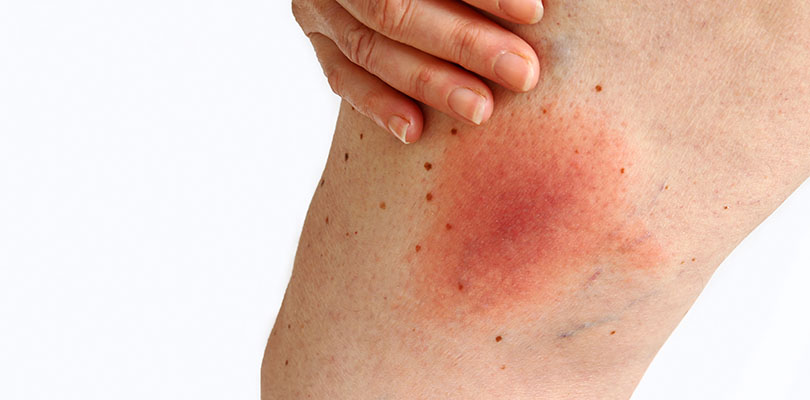
The most common symptom of DVT is calf pain and swelling of the affected leg. It’s rare that both legs will be swollen at the same time. Your leg may feel painful or tender when you stand, move, or touch it. The pain usually starts in the calf and feels like a cramp; it may get worse over time or the pain can become constant. Your leg will feel warm and appear discolored, looking redder than your other leg. If you are experiencing these DVT symptoms and signs in your leg, seek immediate care from a doctor.
Here are a couple other things to note about the symptoms of DVT:
- A small blood clot may not cause symptoms
- Years after DVT, up to 20% of patients may develop post-thrombotic syndrome. This syndrome has symptoms of leg swelling, heaviness, pain and skin changes, which cause pressure related complications. Post-thrombotic syndrome is the result from obstructed deep veins.
Venous thromboembolism treatment focuses on preventing blood clots in those who may have a deep vein thrombosis or a pulmonary embolism.
Warning Signs of Pulmonary Embolism
In some cases, a pulmonary embolism is the first sign of DVT. Make sure you know the warning signs:
- Sudden shortness of breath
- Taking a deep breath or coughing worsens chest pain or discomfort
- Increased heart rate
- Feeling lightheaded or dizzy
- Coughing up blood
Testing for Deep Vein Thrombosis
The most common test for DVT is a duplex ultrasound. The ultrasound shows a visual of the veins of the leg where a doctor can determine whether or not a blood clot is present. Other tests to diagnose DVT are rarely used, but can include a CT scan, MRI and contrast venography. A D-dimer test is a blood test that may be ordered, and a negative test means that you do not have DVT. A positive or high value D-dimer test has multiple causes and requires further testing to reach a DVT diagnosis. If a doctor tests you for a pulmonary embolism, they will commonly use a CT scan to make their diagnosis.
Treatment of Deep Vein Thrombosis
Treatment is crucial to minimize the chance that a piece of a blood clot might break loose and flow into the lungs. Treatment usually involves taking blood thinners for at least three months to prevent existing clots from growing. Blood thinners reduce the risk of blood clots and the main prescriptions are heparin (given intravenously or as an injection) and warfarin (an oral pill). Surgical treatment is available, but rare. Surgery is used to remove a clot when the clots cause so much back pressure in the leg that the tissues do not receive an adequate amount of oxygen and nutrients.
How to Prevent Deep Vein Thrombosis
There are some actions you can take to minimize your risk of contracting DVT. Some preventative measures include:
- Elevating your legs when possible
- Avoiding sitting still and making sure to take walks throughout the day since exercise lowers your risk of blood clots
- When sitting, not crossing your legs, as it obstructs blood flow
- Wearing compression stockings
- Moving as soon as possible after bed rest or surgery (as long as it is safe to do so)
- Make lifestyle changes like losing weight or quitting smoking
- Stopping on road trips to walk around
- Standing or moving your legs occasionally on a plane (there are some airplane exercises that can be found online)
Find out your family history to see if there are blood clotting issues that may have been passed down in your DNA. If you know whether you are at risk for DVT, you can take preventative measures to avoid these serious blood clots.