Candida Auris
It’s important to inform yourself about Candida auris because it presents a global health threat. Candida auris has been described as a superbug because it is resistant to multiple antifungal drugs, difficult to identify, and has caused outbreaks in healthcare settings, affecting hospital patients as a result.
What Is Candida Auris?
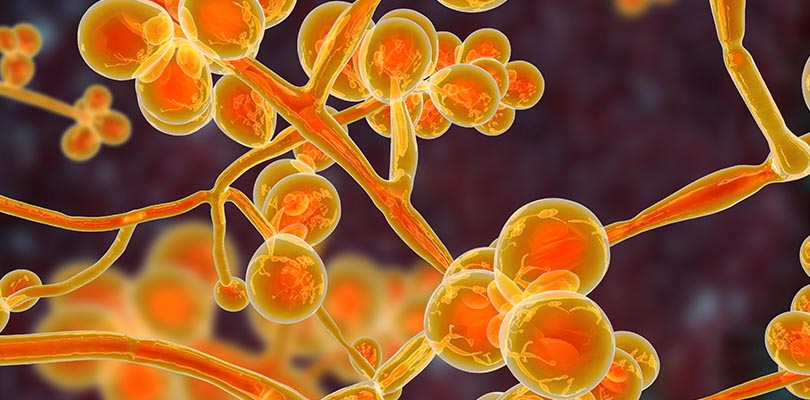
While Candida auris has been misidentified as a bacterial infection, it’s actually a fungus – a type of yeast to be more accurate. The Candida species has generally been known to cause vaginal and skin infections (aka yeast infections), but rarely causes serious illness.
Candida auris, on the other hand, is more dangerous because the fungus can enter the bloodstream and spread throughout the body to cause invasive infections. This yeast can live on the skin or other body parts without making a person sick, but a Candida auris infection can affect any part of the body. Candida auris has caused severe illness in hospital patients, who are more vulnerable to infections.
Where did Candida Auris Come From?
These infections have started appearing all over the globe, rather than spreading from one region to another systematically.
The Candida auris organism was discovered in 2009 in the ear of an elderly woman in Japan, but strains were present in Pakistan and India years prior.
The infection appears to have emerged independently on different continents at the same time, which is concerning for the Centers of Disease Control and Prevention (CDC).
Candida Auris Causes
An article from the American Society for Microbiology proposes that Candida auris is a new type of pathogenic fungus that is the result of human-induced global warming.
Humans have caused changes to the environment, which may have helped cause the sudden emergence of Candida auris infections around the globe. Global warming, however, may only be part of the reason that Candida auris has become known as a superbug.
There are a few other ways that researchers speculate that the infections spread:
- A person comes into contact with contaminated surfaces in the environment
- The infection passes between patients via direct contact
The CDC continues their research on the spread of Candida auris, especially since some folks may be carriers for many months and be unaware that they are passing the fungus along to others.
Candida Auris Symptoms
The time it takes for symptoms to appear likely varies from patient to patient. The fungus may infect different parts of the body with different symptoms in each individual. The symptoms of Candida auris infection depend on the affected body part. Some symptoms include:
- Fever and chills (common in bloodstream infections)
- Sepsis
- Little or no improvement with conventional antifungal therapy
- Coma and organ failure if treatment is delayed
If the affected individual is a hospital patient, symptoms may not be noticeable because they are generally already sick and have other symptoms that mask Candida auris symptoms.
What Type of Infections Can Candida Auris Cause?
The types of infections that Candida auris can cause are mainly bloodstream, wound, and ear infections. These infections are difficult to treat because they are often resistant to medication. Invasive infections can be fatal, so it’s extremely important to seek medical intervention as early as possible.
DNA testing kits can help delve into your ancestry and identify whether you have genes that may increase the chance of developing specific health issues.
Who Is at Risk for Candida Auris?
These fungal infections have affected all age groups. Many diagnosed cases of Candida auris have occurred in medical centers, nursing homes, and long-term care facilities among affected people who were already diagnosed with another illness. Those who are at the highest risk for infection include:
- Those who have had frequent hospital stays or those with weakened immune systems from conditions like blood cancers or diabetes
- Hospital patients that have been in a healthcare facility a long time
- Those who have a catheter or other tubes entering their body
- Those who have previously received antibiotics or antifungal medication
How Is Candida Auris Diagnosed?
More than a third of people with Candida auris infections die within a few months because it can be difficult to identify quickly. As unsettling as it is, Candida auris is often multi-drug resistant, so it doesn’t respond to several antifungal drugs used to treat Candida infections.
Candida auris is also challenging to identify with standard laboratory methods, so specialized testing is required. Lab testing on blood cultures or other specimen is needed to confirm the diagnosis. The GenMark ePlex Blood Culture Identification Fungal Pathogen Panel is the first FDA-approved molecular test to identify Candida auris. Candida auris can be misidentified in labs without the specific technology, and this misidentification can lead to improper treatment management.
Treatment for Candida Auris
Treatments for Candida auris are severely limited. Infections caused by Candida auris are difficult to treat because the fungal infection doesn’t respond to commonly used antifungal drugs. There are only a few medications available to treat fungi, for example, medications like echinocandins.
Some strains of Candida auris are resistant to all three major classes of antifungal drugs (azoles, polyenes, and allylamine/thiocarbamates), which makes treating the infections even more difficult.
There are some preventative measures you can take to avoid infections in general. These actions include:
- Washing your hands
- Staying up to date on your vaccinations
- Avoiding people who are sick with something contagious
- Using an alcohol-based hand sanitizer
- Regular cleaning and disinfecting of the environment around you
Most people who carry the fungus do not get sick from it. Candida auris has not spread to wide numbers of the general population, and healthy people rarely develop the infection. Make sure that you take the appropriate preventative action to stay on top of your health and consult your doctor with any health concerns.